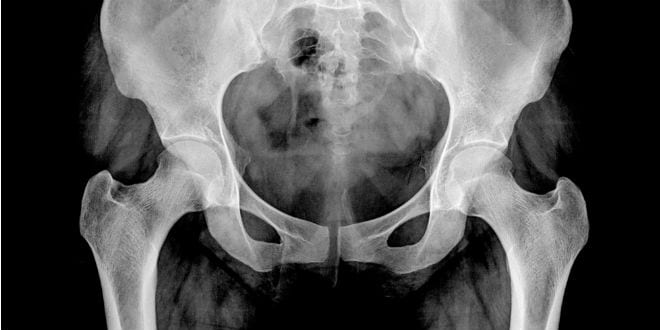
Despite the openness of today’s world, there are medical conditions that people don’t like to mention or problems about which they know little despite their suffering. One such condition is pelvic floor prolapse, from which a third of women suffer over their lifetimes.
“Pelvic floor” refers to a group of muscles that form a kind of hammock across the female pelvic opening. Normally, these muscles and the tissues surrounding them keep the pelvic organs – bladder, uterus, vagina, small bowel and rectum – in place. “Prolapse” is a descending or drooping of organs.
Women may develop pelvic floor problems in these muscles and tissues – mostly commonly following childbirth – and as they get older, pelvic organ prolapse and other pelvic floor disorders become more common. In Israel and many other countries, women of any age aren’t very aware of such difficulties, but in others – Brazil, for example – women who have not developed weak pelvic floors often undergo preventive surgery to keep the organs in place.
There are ways to prevent pelvic floor prolapses: These include doing Kegel exercises (repeated contraction of muscles in the pelvic area to strengthen the muscles, or mechanical treatments, such as inserting a small plastic device called a pessary to provide support for drooping organs. In addition, maintaining a healthy weight and not smoking are important.
Symptoms of the condition include a feeling of pressure or fullness in the pelvic area; a backache in the lower back; urinary problems such as the leaking or urine or a chronic urge to urinate; and painful intercourse.
Prolapse can occur when something – such as pregnancy, labor and childbirth (the most common causes), obesity, constipation, hysterectomy (surgical removal of the uterus) or cancer in the pelvic organs – creates pressure in the abdomen. Having a first-degree relative with pelvic organ prolapse also increases the risk.
Obstetricians and gynecologists have long blamed having five or more pregnancies/deliveries, which they scientifically call “grand multiparity.” Multiparous women have a risk 1.5 times more of pelvic floor prolapse than women who have had fewer pregnancies and deliveries.
They also thought that having a cesarean section to deliver the babies reduces the risk of pelvic floor prolapse because less pressure is put on the internal organs in the abdomen.
But a leading Israeli ob/gyn has found that this is not necessarily true Prof. Eyal Sheiner, head of the obstetrics/gynecology department B at Soroka University Medical Center in Beersheba, Israel, has just disclosed the results of a study he and his team have conducted on the subject.
In this study, the team examined whether an emergency cesarean procedure performed during normal labor after a long time of trying unsuccessfully to push the baby out also had a protective effect against future pelvic floor dysfunction. Their study has just earned them a best-poster award at this year’s Conference of the Israel Society for Maternal and Fetal Health. They will also write a medical journal article on the subject, as it is certain to interest their fellow specialists.
It can be concluded that the known protective effect of cesarean section on pelvic floor dysfunction later in life takes place as long as the operation is performed before the final stage at birth. If the woman’s uterus is surgically opened to remove the baby after this final stage in delivering vaginally is not successful, then cesareans do not reduce the risk of pelvic floor problems.
Cesareans are necessary if the final stage of vaginal birth is not getting anywhere because of difficulty in moving the baby’s head in the mother’s pelvis because of its size or position or fetal distress.
The team studied the records of all women who gave birth at Soroka between 1991 and 2017 – 106,000 cases. These included numerous multiparous women, many of them ultra-Orthodox Jews and Bedouin women, who have large families.
The cases were divided into three groups – women who gave birth in a normal birth; those who had a planned cesarean section and did not try to have a vaginal birth first; and third group who had to have a cesarean after unsuccessfully trying to give birth normally. A comparison was made among the groups related to pelvic floor dysfunction and pelvic floor repair.
A total of 86.7% underwent a normal childbirth, 11.7% had a planned cesarean section, and 1.7% had at least one cesarean section after a prolonged pushing stage.
The incidence of pelvic floor dysfunction among the women included in the study was 0.7% (719 women), and the rate of hospitalizations for surgical repair of pelvic floor dysfunction was significantly lower among women who gave birth vaginally compared with women who had a cesarean section after a failed vaginal birth.
It became clear that cesareans offered no protection against pelvic floor dysfunction in the third group
Sheiner, who graduated from Ben-Gurion University of the Negev in Beersheba, told Breaking Israel News that the study did not result in policy changes. In any case, Soroka does not use forceps to deliver babies because they can cause harm to the babies and their mothers, but it does sometimes do vacuum deliveries to release the baby.
The cesarean rate is 17% – among the lowest in the country – at the Beersheba hospital, he said proudly, and the rate of urgent cesareans is even lower – 5%. “We warmly recommend vaginal births whenever possible, as it is safer for both mother and baby in most cases and presents the fewest complications.